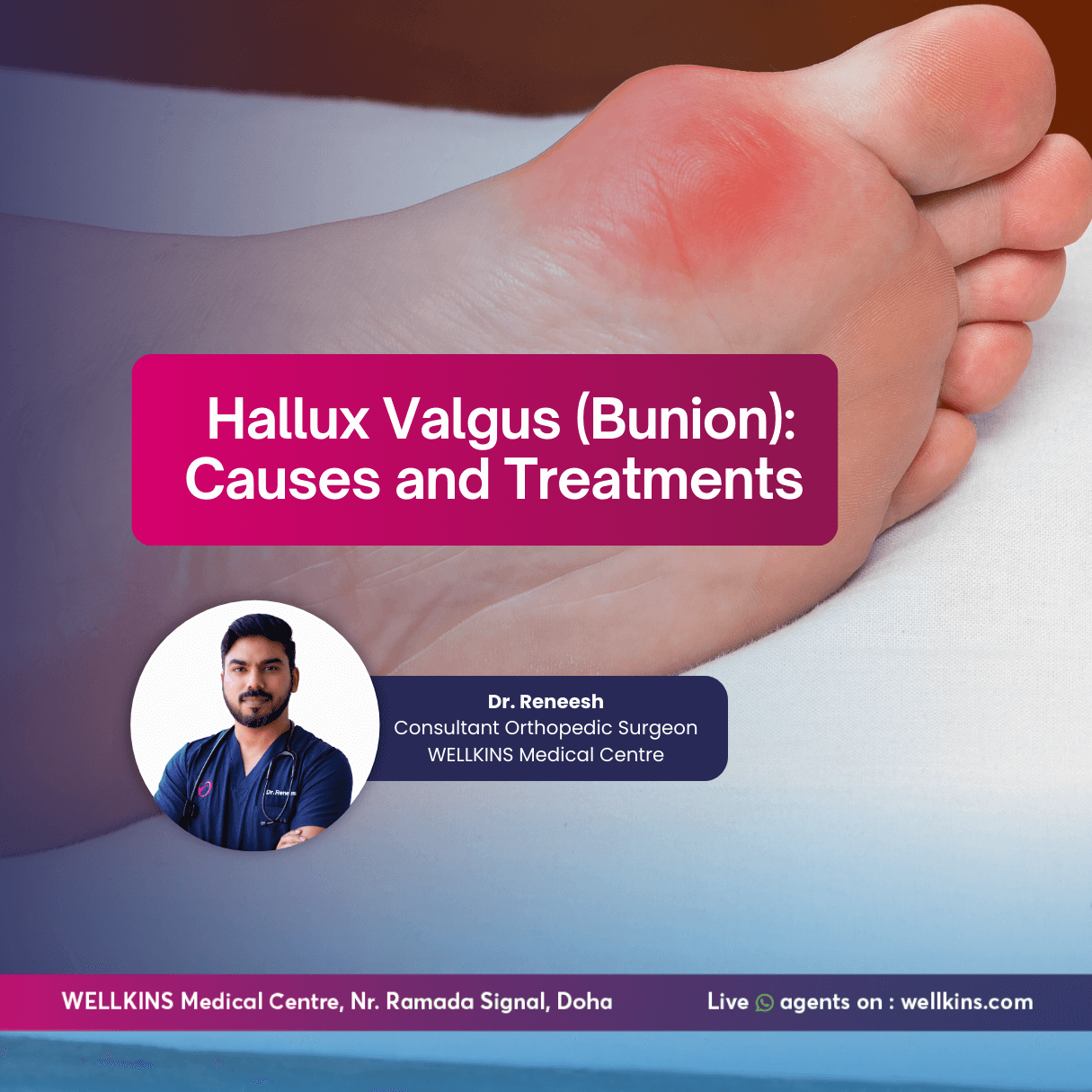
Author: Dr. Reneesh (Consultant Orthopedic Surgeon – Wellkins Medical Centre)
Introduction
Hallux valgus, commonly known as a bunion, is a progressive forefoot deformity characterized by lateral deviation of the great toe (hallux) and medial prominence of the first metatarsal head. It is one of the most frequently encountered foot deformities in orthopedic practice and can significantly affect gait, footwear tolerance and quality of life. At Wellkins Medical Centre, we see patients from all walks of life from athletes to corporate professionals who often mistake this structural bone change for a simple callus or skin growth. Although often perceived as a cosmetic issue, hallux valgus is a biomechanical disorder that may lead to chronic pain, secondary deformities and functional limitation if left untreated. It represents a subluxation (partial dislocation) of the joint, meaning the bones have shifted out of alignment. Early identification and appropriate management are essential to prevent progression and complications.
For individuals experiencing bunion (hallux valgus) in Qatar, early recognition and appropriate care are key to reducing pain and preventing progression. From a clinical perspective, bunions develop due to structural foot changes influenced by footwear, biomechanics and genetic factors. Symptoms such as toe deviation, joint inflammation and difficulty with walking require timely assessment. Effective treatment focuses on relieving pressure, improving foot alignment and restoring function through proper footwear guidance, orthotic support, targeted exercises and, when necessary, medical or surgical intervention aimed at long-term foot health rather than temporary relief.
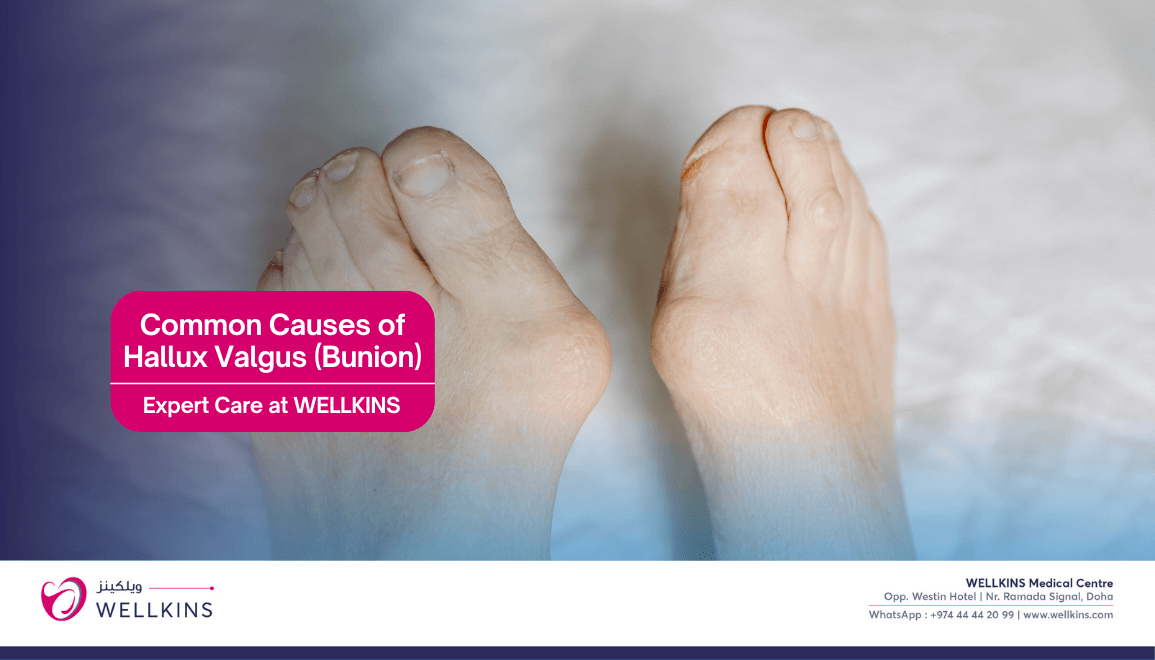
Hallux valgus is a multifactorial condition resulting from a combination of intrinsic (biological) and extrinsic (environmental) factors. It is rarely caused by a single event but rather a slow “drift” of the bone structure over years.
Common causes include:
- Genetic predisposition: A positive family history is one of the strongest predictors; you likely inherited the foot type prone to bunions.
- Foot biomechanics abnormalities: Such as flatfoot (pes planus), low arches and excessive pronation which place uneven pressure on the big toe joint.
- Ill-fitting footwear: Particularly narrow, tight, or high-heeled shoes that squeeze the toes into an unnatural “V” shape.
- Ligamentous laxity: Naturally loose ligaments or connective tissue weakness (often seen during pregnancy or in specific syndromes).
- First ray instability: Hypermobility of the joint that allows the first metatarsal to swing outward too easily.
- Inflammatory conditions: Such as rheumatoid arthritis, which can degrade the joint surfaces.
- Neuromuscular disorders: Conditions that affect muscle balance in the foot.
- Occupational factors: Jobs requiring prolonged standing or the use of restrictive safety boots.
Symptoms
Symptoms of hallux valgus vary depending on the severity and stage of the deformity. It is important to note that the size of the bunion does not always correlate with the level of pain; some small bunions are very painful, while some large ones are asymptomatic.
Patients may present with:
- Medial prominence: A visible “bump” on the inside of the foot at the base of the big toe.
- Pain and tenderness: Especially localized over the bunion, aggravated by tight shoe wear or long walks.
- Inflammation: Redness, swelling, or callus formation over the medial eminence (the bump).
- Toe deviation: The great toe begins to angle toward the second toe, sometimes even overlapping or “diving” under it.
- Restricted movement: Stiffness or painful “grinding” in the first metatarsophalangeal (MTP) joint.
- Difficulty with footwear: Finding that shoes which used to fit are now too narrow or cause blistering.
- Altered gait: Shifting weight to the outside of the foot to avoid big toe pain, which can lead to discomfort in the “ball” of the foot (transfer metatarsalgia).
Diagnosis
Diagnosis at Wellkins Medical Centre begins with a physical evaluation by an orthopedic surgeon. We don’t just look at the toe; we look at how the entire foot functions as a unit.
- Inspection: Checking for hallux deviation, bunion size and skin changes like corns or ulcers.
- Palpation: Testing for tenderness, signs of bursitis (fluid sacs), or hardened callosities.
- Range of Motion: Assessing how well the joint moves and checking for early signs of arthritis.
- Alignment Evaluation: Checking arch height, ankle flexibility and gait (how you walk).
- Secondary Checks: Identification of associated deformities such as hammer toes or claw toes on the smaller digits.
Radiological Evaluation
Weight-bearing radiographs (X-rays taken while standing) are the gold standard for confirming diagnosis and planning treatment:
- Hallux Valgus Angle (HVA): Measuring the degree of deviation of the big toe.
- Intermetatarsal Angle (IMA): Measuring the spread between the first- and second foot bones.
- Distal Metatarsal Articular Angle (DMAA): Checking the tilt of the joint surface.
- Joint Congruency: Assessing if the joint is still “seated” properly or if degenerative changes (arthritis) have begun.
Complications
Untreated or progressive hallux valgus may lead to several complications that extend beyond the big toe itself, affecting the entire kinetic chain of the lower limb.
- Chronic pain: Persistent inflammation that can make even simple standing difficult.
- Bursitis: The formation of a painful, fluid-filled sac over the medial eminence due to constant friction.
- Degenerative arthritis: Permanent wear and tear of the cartilage in the first MTP joint.
- Transfer metatarsalgia: Pain in the second or third toe joints because the big toe is no longer carrying its fair share of the body’s weight.
- Secondary toe deformities: The big toe pushing against the others can cause hammer toes, claw toes, or painful corns.
- Reduced mobility: A gradual withdrawal from exercise and social activities due to foot discomfort.
- Impaired balance: Especially in elderly patients, bunions can increase the risk of falls due to instability.
Prognosis
The prognosis of hallux valgus depends on the severity of deformity, symptom duration, and patient compliance with lifestyle changes. While a bunion will not “un-bend” on its own, its progression can often be slowed or managed effectively. Mild to moderate cases often respond well to conservative management aimed at symptom relief and joint preservation. Progressive or severe deformities, especially those causing “crossover toe,” may require surgical correction. With appropriate procedure selection and adherence to postoperative rehabilitation, surgical outcomes are generally favorable, with high patient satisfaction and functional improvement.
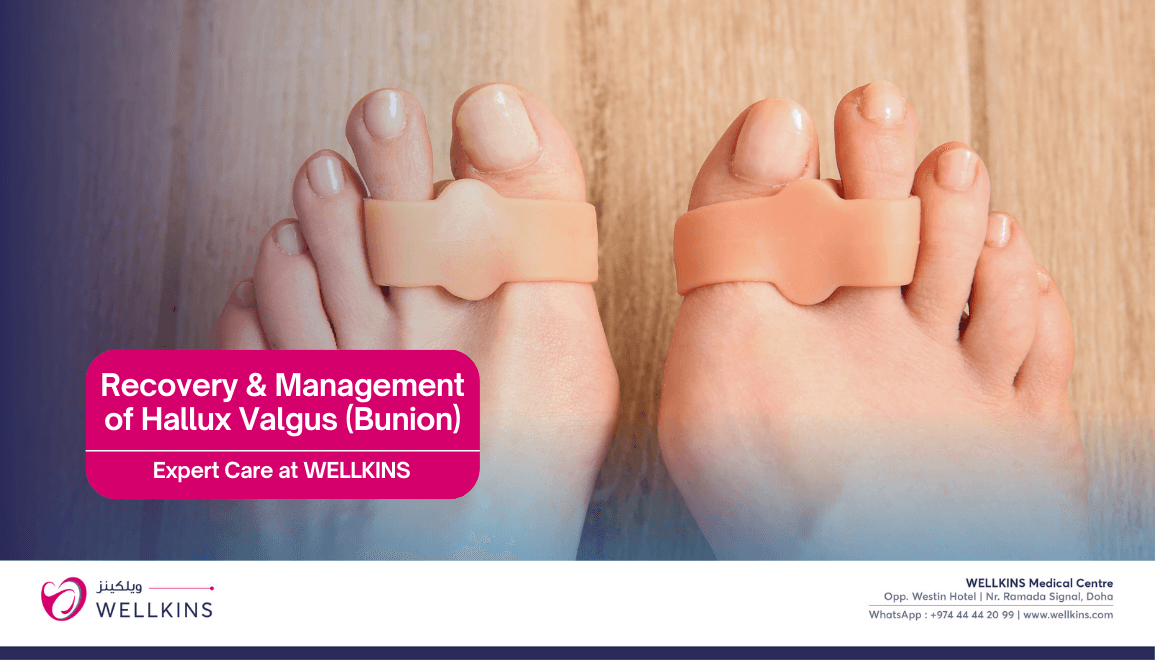
Recovery and Management
Non-surgical management is the first line approach for most patients at Wellkins Medical Centre and focuses on symptom control and preventing the deformity from worsening.
- Footwear modification: Switching to shoes with a wide, deep toe-box and soft uppers.
- Orthotic insoles: Custom or medical-grade inserts to support the arch and correct over-pronation.
- Bunion pads/Silicone spacers: To reduce friction against shoes and keep the toes slightly separated.
- NSAIDs: Medications to manage acute pain and “flare ups” of inflammation.
- Activity modification: Choosing low-impact exercises (like swimming or cycling) during painful periods.
- Physical Therapy: Strengthening the intrinsic muscles of the foot to provide better dynamic support.
Surgical Management
Surgery is indicated for patients with persistent pain and functional limitation despite adequate conservative treatment. Modern bunion surgery is highly sophisticated, focusing on realigning the bone rather than just “shaving off the bump.”
- Osteotomy: Precisely cutting and shifting the bone into a straighter position, secured with tiny screws.
- Soft tissue repair: Rebalancing the tendons and ligaments around the joint.
- Recovery timeline: Most patients can walk in a special “post-op shoe” shortly after surgery, but full return to sports or high heels may take several months.
Conclusion
Hallux valgus is a common and often progressive forefoot deformity with both functional and biomechanical implications. It is more than a cosmetic concern; it is a structural issue that can change the way you move through the world. From an orthopedic surgeon’s perspective, early diagnosis, patient education and individualized treatment planning are key to achieving optimal outcomes. At Wellkins Medical Centre, we are dedicated to helping you walk without pain. Whether you need a simple orthotic adjustment or a surgical consultation, our team is here to support your journey back to healthy feet.
To book an appointment at Wellkins Medical Centre: https://wellkins.com/orthopedics/