Author: Dr. Reneesh (Consultant Orthopedic Surgeon – WELLKINS Medical Centre)
Introduction to Plaster Casts
Immobilization is one of the most important principles in orthopedic treatment. At Wellkins Medical Centre, we often tell our patients that while the body does the actual healing, the cast provides the “peace and quiet” necessary for that healing to occur. Whether managing fractures, ligament injuries, or post-operative cases, proper stabilization ensures pain relief, prevents further damage and promotes healing by keeping the affected structures in their optimal biological alignment. Among the various immobilization methods available today, from advanced braces to internal plates, the plaster cast remains a reliable, cost-effective and widely used technique in orthopedic practice. In this article, I will discuss the uses of plaster casts, the types available, the crucial difference between a plaster slab and a plaster cast and the meticulous method we use at Wellkins for application.
For individuals in Qatar with fractures or soft tissue injuries, plaster casting provides essential support by stabilizing the affected limb and maintaining proper alignment during healing. When applied correctly, a plaster cast helps reduce pain, control swelling, protect the injury and promote safe, effective recovery as part of a complete orthopedic care plan.
Uses of Plaster Cast
Plaster casts are versatile tools that serve several critical functions in a patient’s recovery journey:
- Fracture Immobilization: This is the most common use. It maintains bone alignment after “reduction” (setting the bone) to ensure the ends knit back together correctly without deformity.
- Soft Tissue Injuries: For severe sprains, grade-III ligament tears, or tendon ruptures (like the Achilles), movement restriction is mandatory to allow the fibers to heal without being overstretched.
- Post-operative Support: After surgery involving pins, plates, or tendon repairs, a cast acts as a secondary layer of protection against accidental movement or impact.
- Deformity Correction: In pediatric orthopedics, “serial casting” is used to gradually move a limb into the correct position, such as in the treatment of clubfoot (Congenital Talipes Equinovarus).
- Pain Relief: By eliminating movement at the injury site, casts significantly reduce movement-related pain and the painful muscle spasms that often accompany broken bones.
Types of Plaster Cast
Casts are tailored specifically to the injury site. At Wellkins, we choose the cast type based on the need for stability versus the need for functional movement in surrounding joints.
Upper Limb Casts
- Short arm cast: Extends from below the elbow to the knuckles.
- Long arm cast: Extends from the upper arm to the knuckles, keeping the elbow at a 90° angle.
- Thumb spica cast: Specifically stabilizes the thumb and wrist, often used for scaphoid fractures.
- Ulnar/Radial gutter casts: Targeted immobilization for specific finger or metacarpal fractures.
Lower Limb Casts
- Short leg cast: From below the knee to the base of the toes.
- Long leg cast: Extends from the upper thigh to the toes.
- Cylinder cast: Immobilizes the knee while allowing the ankle to move.
- Patellar tendon-bearing cast: A specialized cast that allows for early weight bearing.
- Hip spica cast: Often used in children to immobilize the hip and thigh.
Based on Material
- Plaster of Paris (POP): Made of gypsum-soaked bandages. It offers excellent molding ability (allowing for a “custom fit”) and is economical, though it is heavier and takes about 24–48 hours to fully dry.
- Fiberglass cast: A synthetic alternative that is incredibly lightweight and “breathable.” It sets in minutes and is more durable, though it is less “moldable” than traditional POP.
Plaster Slab vs. Plaster Cast
Although often used interchangeably in casual conversation, these two are structurally and functionally distinct.
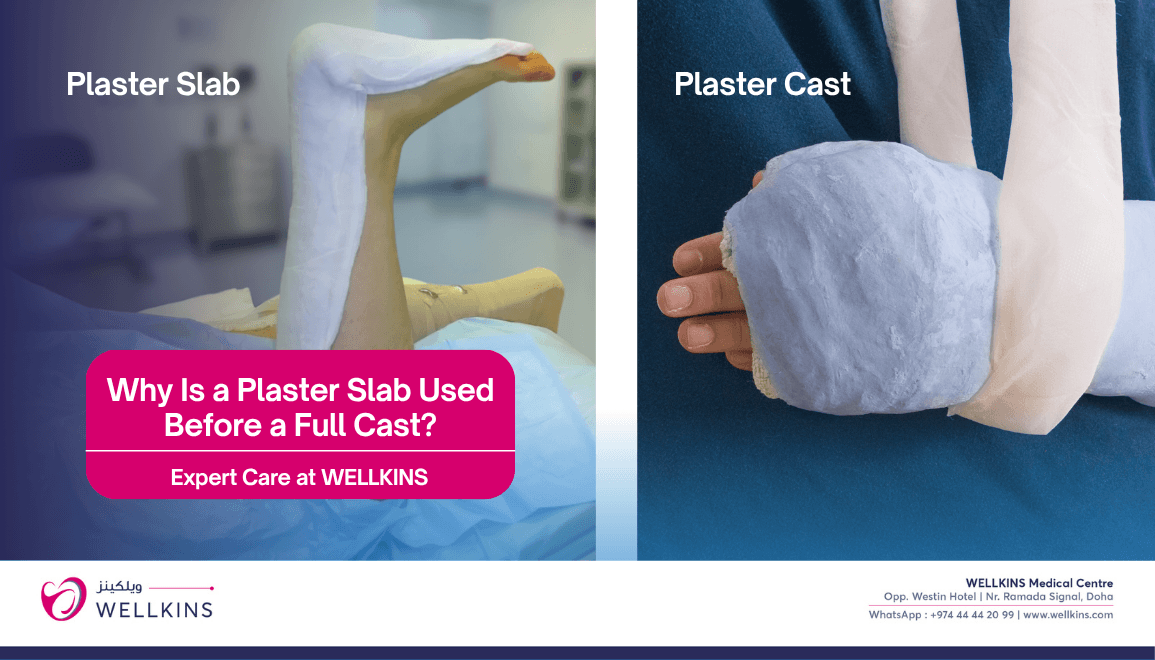
Plaster Slab (Backslab): A plaster slab, also known as a backslab, is a partial cast that supports only one side of the injured limb. It is commonly used in the initial stage of an injury or fracture when swelling is expected, as it allows space for expansion and helps prevent complications. The slab is secured with a bandage rather than being fully enclosed, making it easier to adjust, loosen, or remove if needed. It provides temporary support and partial immobilization while ensuring patient comfort during the early healing phase.
Plaster Cast (Full Cast): A plaster cast is a fully enclosed, circular support that encases the entire injured limb. It is typically applied after the swelling has reduced and is intended for long-term immobilization to promote proper healing of fractures or injuries. The cast is rigid and not easily removable, offering strong stability and complete support to the affected area. Its firm structure helps maintain correct alignment of bones throughout the recovery period.
Plaster Slab (Back Slab)
- Covers only a portion of the limb (usually the back or one side).
- It is not circumferential; it doesn’t go all the way around.
- Secured with a soft elastic bandage.
- Its primary benefit is that it allows room for swelling.
Plaster Cast
- It is circumferential, encircling the entire limb.
- Rigid, stable and provides the strongest form of external immobilization.
- Because it is a closed loop, it does not allow for expansion if the limb continues to swell.
Why is Plaster Slab Used Initially Instead of a Full Cast?
In acute fractures and fresh injuries, the body responds with significant inflammation. Swelling is expected to peak within the first 48–72 hours. If a full circumferential cast is applied immediately, it creates a dangerous “fixed container.”
Risks of an immediate full cast:
- Vascular Compromise: Swelling against a rigid cast can cut off blood flow to the fingers or toes.
- Nerve Compression: Constant pressure can lead to permanent nerve damage.
- Compartment Syndrome: This is a surgical emergency where pressure within the limb rises to a level that destroys muscle and nerve tissue.
A plaster slab is preferred initially because:
- It accommodates the natural “expansion” of the limb during the inflammatory
phase. - It allows the medical team and the patient to monitor the skin and circulation more
easily. - Once the swelling subsides (usually after 3–5 days), the slab is safely replaced with
a definitive full cast.
Plaster Cast Application Technique
Applying a cast is an art form that requires precision to ensure comfort and prevent complications like “cast sores.”
- Step 1: Preparation: We confirm the fracture is in the correct position and place the limb in a “functional alignment” (e.g., the position most useful for the patient during recovery).
- Step 2: Stockinette Application: A soft, tubular cloth is applied directly to the skin to act as a barrier.
- Step 3: Padding: Layers of soft cotton padding are wrapped around the limb. We add extra padding over bony prominences like the wrist bone or ankle to prevent pressure ulcers.
- Step 4: Wetting the Plaster: Plaster rolls are dipped in room temperature water. We gently squeeze out excess water; twisting too tightly can ruin the lamination.
- Step 5: Application: The plaster is rolled on smoothly. We avoid pulling it tight, as the material naturally shrinks slightly as it dries.
- Step 6: Molding: This is the most critical part. The surgeon uses their palms (not fingertips) to mold the cast. Using fingertips can create small indentations that press against the skin and cause sores.
- Step 7: Post-Application Check: We always check for “The 5 P’s”: Pain, Pallor (color), Pulselessness, Paresthesia (sensation) and Paralysis (movement).
Conclusion
Plaster casting remains a cornerstone in orthopedic fracture management, providing essential immobilization to support proper bone healing. Understanding the distinction between a plaster slab and a plaster cast is critical, particularly in the acute injury phase when swelling is at its peak. While it might seem like “just a bandage,” the initial use of a slab is a vital safety measure that allows room for swelling, reduces the risk of complications and protects the injured limb during the early stages of recovery.
At Wellkins Medical Centre, we ensure that every cast is applied with meticulous care, guided by clinical assessment and patient comfort. Our approach focuses not only on stabilizing the fracture, but also on monitoring circulation, minimizing stiffness and planning timely follow up. This attention to detail supports optimal healing and helps patients return to normal function safely and confidently.
To book an appointment at Wellkins Medical Centre: https://wellkins.com/orthopedics/